Practice makes progress: evidence, experience, and expectations in rehabilitation design
An evidence-based approach is “the conscientious, explicit, and judicious use of the current best evidence in making decisions about the care of individual patients”(1). It represents the aim of Sports and Exercise Medicine (SEM) practice. The hierarchy of scientific evidence for health research ranks different types of evidence. It suggests that where possible, we should use interventions that demonstrate effectiveness in meta-analysis or systematic reviews, or at the very least, a randomized controlled trial.
However, evidence-based practice has its roots in medicine, and medical research is commonly binary. For example, researchers typically design studies to establish the efficacy of a particular treatment compared to a control group (no intervention) or to compare different treatment options.
THE SCIENCE-PRACTICE GAP Injury rehabilitation is different from clinical medicine, and professionals working in these spaces generally aren’t presented with binary choices. Practitioners have the option to choose between and combine multiple therapies—for example, acute injury management with ice, elevation, and immobilization or early mobilization and loading. Adjunctive therapies offer other treatment options, for example, manual therapy, ultrasound, laser, dry needling, cupping, shockwave therapies, and exercise prescription. Exercise prescription alone presents many adjustable parameters (frequency, volume, velocity, and intensity) that will influence treatment outcomes. While each aspect of treatment may have supporting scientific evidence, it is rare for research to investigate the interactions of different therapies that could reasonably complement each other. The ‘science-practice gap’ is the disparity between research results and their applicability in clinical practice. A six-step plan may address the development of evidence-informed rehabilitation, which narrows the gap between the evidence base and clinical practice.
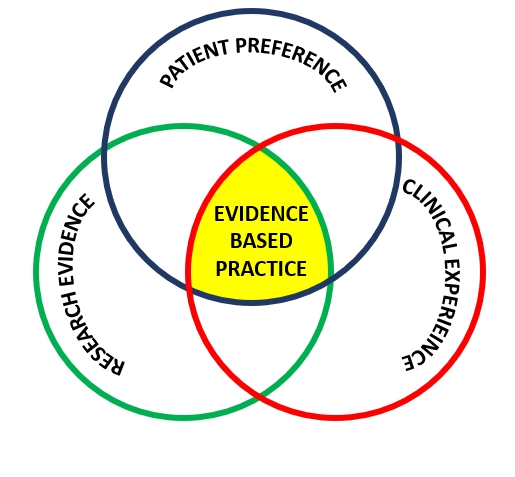
EVIDENCE-BASED PRACTICE To narrow the ‘science-practice gap,’ medical researchers advocate for evidence-based practice that increases scientific research awareness, interpretation, and implementation by healthcare professionals. However, practitioners need to apply the knowledge appropriately in their clinical context using clinical experience and understanding athlete preferences (see figure 2). For example, blood flow restriction (BFR) therapy could help maintain muscle mass and strength in an athlete with a long-term lower limb injury. However, clinical experience identifies that although BRF allows for muscular metabolic stress at lower loads, it is often difficult for athletes to tolerate. As a result, practitioners may need to use alternative treatment modalities despite the evidence base to support BFR. Thus, evidence-based practice is not the selection of treatment modalities supported by evidence but rather appropriate clinical reasoning to identify the athlete’s most appropriate holistic treatment modality.
To read the full article visit - https://www.sportsinjurybulletin.com/improve/improve/practice-makes-progress-evidence-experience-and-expectations-in-rehabilitation-design